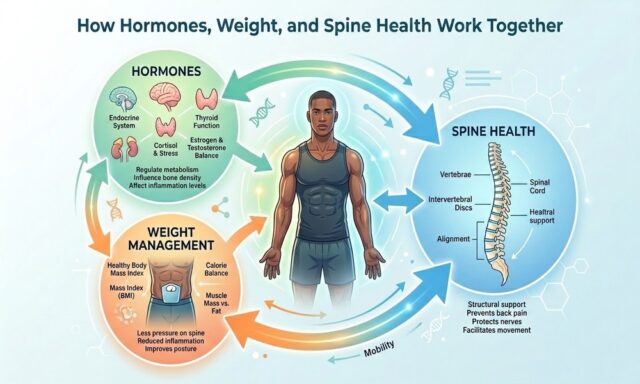
Chronic pain and limited mobility rarely come from just one cause. More often, they develop through a mix of issues that build over time. Three of the most overlooked factors are hormonal imbalance, weight gain, and spinal stress. Each can affect the others, creating a cycle that becomes harder to break the longer it continues.
Understanding how these systems work together can help people spot early warning signs and take practical steps to protect their long-term health. This article explores the connection between hormones, body weight, and spine health, and why addressing them together can make a meaningful difference in overall well-being.
The Role of Hormones in Physical Health
Hormones act as the body’s internal messaging system. They help regulate metabolism, energy levels, muscle growth, and the body’s response to stress and inflammation. When hormone levels are balanced, these processes tend to run smoothly. When they are not, subtle changes can start to show up.
For example, declining testosterone or thyroid hormone levels can contribute to fatigue, reduced muscle mass, and a slower metabolism. At first, those changes may seem minor. Over time, though, they can affect posture, strength, and day-to-day function. The body may also become less efficient at repairing itself, which can increase the risk of pain and injury.
Hormonal imbalances can also influence how the body stores fat. Changes in insulin sensitivity or cortisol levels may encourage weight gain, especially around the abdomen. That extra weight does more than affect appearance. It can place additional strain on the joints and spine, increasing the likelihood of discomfort and reduced mobility.
The Connection Between Hormones and Weight Regulation
Hormones play a central role in weight regulation. When hormone levels shift, the body’s ability to burn calories, build muscle, and manage appetite can change in noticeable ways.
For example, lower testosterone levels in men are often associated with increased fat accumulation and reduced lean muscle mass. That combination can slow metabolism, making weight gain easier and weight loss more difficult. Elevated cortisol levels linked to chronic stress may also encourage fat storage and increase cravings for calorie-dense foods.
In clinical settings, including specialized TRT treatment centers such as Lions OpTimal Health, hormone therapy is often approached as one part of a broader, individualized care plan. According to Lions OpTimal Health, hormone replacement therapy is typically guided by both symptom patterns and laboratory findings, with the goal of restoring physiological balance rather than using a one-size-fits-all approach. When hormone levels are managed appropriately, some individuals may notice improvements in energy, body composition, and overall metabolic function, which can support more sustainable weight regulation over time.
How Weight Gain Impacts the Spine
Weight gain is not only a metabolic concern. It also has direct mechanical effects on the body, especially the spine. The spine is built to support body weight and allow movement, but it still has limits. When excess weight is added, those limits are pushed.
Carrying extra weight increases pressure on the intervertebral discs, particularly in the lower back. Over time, that pressure can contribute to disc degeneration, inflammation, and nerve compression. These changes often lead to chronic back pain or stiffness that worsens with activity.
Weight gain can also affect posture. Extra abdominal weight tends to pull the body forward, increasing the curve of the lower spine. That shift forces surrounding muscles to work harder to maintain stability, which can lead to fatigue, muscle tension, and ongoing discomfort.
Chronic Inflammation and Pain Signals
Inflammation is another major link between hormones, weight, and spinal health. Short-term inflammation is part of the body’s natural healing process. Chronic inflammation, however, can contribute to persistent pain and tissue damage.
Excess body fat, particularly visceral fat, releases inflammatory chemicals that circulate throughout the body. These chemicals can affect the joints, muscles, and spinal discs, increasing sensitivity to pain. Hormonal imbalances can make the problem worse by disrupting the body’s natural anti-inflammatory mechanisms.
As a result, even relatively minor spinal issues can feel more intense. What starts as occasional discomfort may gradually develop into ongoing pain that interferes with daily life. Addressing inflammation often calls for a mix of lifestyle changes, medical support, and consistent monitoring.
Weight Management as a Component of Pain Relief
Managing weight is often an important step in reducing spinal stress and improving mobility. Even modest weight loss can lower pressure on the spine and improve overall function.
In structured care settings, including weight loss programs like those at EveresT Men’s Health, weight management is treated as a medically supervised process rather than a short-term fix. That may include nutritional guidance, exercise planning, and clinical evaluation to identify underlying contributors such as metabolic changes or hormonal imbalances that may be affecting body weight.
This kind of oversight can help ensure that weight loss strategies are safe and aligned with an individual’s broader health profile. It also reinforces an important point: weight gain is not always driven by lifestyle habits alone, but can also be influenced by underlying physiological factors.
Sustainable weight loss can lead to noticeable improvements in pain levels and energy. As the body becomes lighter and more balanced, movement often feels easier, which can encourage more activity and support long-term musculoskeletal health.
Muscle Loss, Stability, and Spinal Support
Muscle mass plays a major role in protecting the spine. Strong core and back muscles help distribute weight evenly and reduce strain on spinal structures. When muscle mass declines, the spine loses part of that support system.
Hormonal imbalances can speed up muscle loss. Reduced testosterone or growth hormone levels can make it harder to maintain strength, even with regular activity. As muscles weaken, the spine may become more vulnerable to misalignment and injury.
This loss of stability can also affect balance and coordination. Small movements that once felt effortless may begin to take more effort, increasing the risk of strain. Over time, this can create a cycle in which pain leads to less activity, and less activity leads to further muscle loss.
Structural Spine Health and Medical Evaluation
Lifestyle factors matter, but structural issues within the spine should not be overlooked. Conditions such as herniated discs, spinal stenosis, and degenerative disc disease may require professional evaluation.
An experienced orthopedic spine doctor, such as CalSpine MD, can assess spinal alignment, identify areas of damage, and recommend appropriate treatment options. These may include physical therapy, noninvasive interventions, or more advanced procedures when needed.
Understanding the spine’s structural condition helps make treatment plans more precise and effective. It can also prevent smaller issues from progressing into more serious problems that may limit mobility over time.
Preventive Care and Long-Term Health Monitoring
Preventive care plays an essential role in maintaining balance across hormones, weight, and spine health. Regular checkups can help identify changes early, before they develop into more serious concerns.
At facilities like Forever Young (fygulfcoast.com), preventive services such as annual wellness visits and chronic disease management can help track key health indicators. Monitoring hormone levels, weight trends, and musculoskeletal health allows providers to make timely adjustments to care.
This proactive approach can lower the risk of chronic pain and improve overall quality of life. It shifts the focus from reacting to symptoms to maintaining stability and preventing decline.
The Cycle of Pain, Inactivity, and Decline
One of the hardest parts of chronic pain is the cycle it can create. Pain often leads to reduced activity, which can contribute to weight gain and muscle loss. Those changes then place more strain on the spine, leading to even more pain.
Breaking that cycle usually requires a broader approach. Addressing only one factor, such as pain relief alone, may provide temporary improvement without resolving the underlying causes. A more effective strategy looks at hormones, weight, and structural health together.
Small, consistent changes can make a real difference. Gradually increasing activity, along with medical support and lifestyle adjustments, can help restore balance and improve function over time.
Conclusion
Hormones, weight, and spine health are closely connected. A change in one area often affects the others, creating a chain reaction that influences how the body feels and functions. Chronic pain and reduced mobility are often the result of this interaction, not a single isolated issue.
By understanding these connections, individuals can take a more informed approach to their health. Supporting hormonal balance, maintaining a healthy weight, and protecting spinal health can work together to reduce pain and improve quality of life over the long term.